For Healthcare Providers
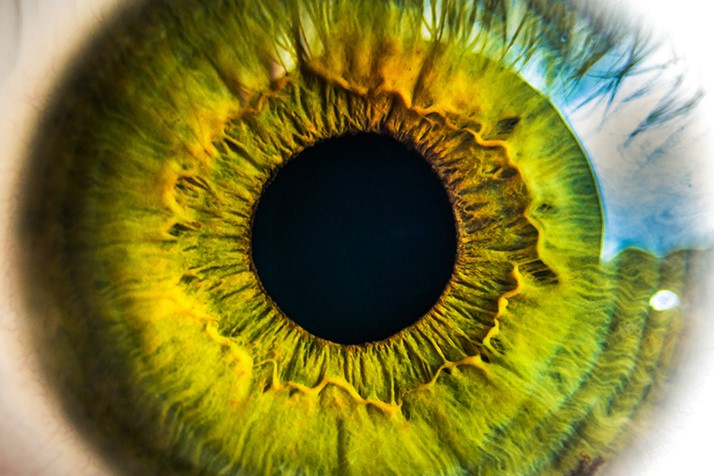
Macular telangiectasia type 2 is a rare disease of the retina that leads to a gradual loss of central vision. MacTel is estimated to affect about 0.1% of the population, and its onset is age-related. Affected individuals are typically diagnosed in their 40s and 50s. MacTel is sometimes mistaken for age-related macular degeneration, due to similar patterns of neovascularization in both diseases. MacTel is a bilateral disease. Fellow eyes are usually similarly affected by the disease, showing the same pathological features. However, the disease may progress at a different rate in each eye.
The retinal alterations caused by MacTel usually begin in a temporal paracentral area. Retinal changes are most pronounced on the temporal side of the retina. Microperimetry and OCT studies to assess function and structure, respectively, suggest that the area temporal to the fovea can be considered the epicenter of disease.
As MacTel progresses, it may encompass an oval region with a radius of about 6⁰ horizontally and 5⁰ vertically, centered on the foveola. Alternatively, MacTel may affect a circular region of the retina, centered on the foveola. MacTel may also be restricted to the temporal macula, leaving the nasal side mostly unaffected.