What To Expect in a MacTel Imaging Exam
April 29, 2024
The following information was sent out via email to people who registered in the LMRI Contact Database.
This post will explain some (but not all) of the imaging exams that your eye doctor may perform during a screening or follow up visit for MacTel, and possible results of those tests. Further tests, not described here, may be performed at your doctor’s discretion.
Before the images are taken, your pupils will be dilated using dilating eye drops. A basic eye exam (called slit-lamp biomicroscopy) will be performed, looking at different parts of your eye, including the back of your eye (your fundus). This is an eye exam you have likely received as part of a routine appointment with an ophthalmologist or optometrist, where you rest your chin and forehead on the device while the doctor looks through the microscope and shines a light on your eye. After examining the front of the eye with the slit lamp, the doctor will examine the back of the eye, looking for any visible changes to the retina (the innermost, light-sensitive layer of tissue of the eye). In a MacTel patient, they might see:
– Changes in retinal transparency (“grayish areas”)
– Crystals (small yellow or white crystal-like deposits in the retina)
– Changes of small retinal vessels (abnormally shaped, dilated vessels, called “telangiectasia”)
– Accumulation of pigment (seen as dark, brownish lesions in the retina) see Figure 1
– Rarely, neovascularization (newly formed, leaky, pathological vessels) and/or bleeding can be found.
The changes are usually limited to a central, oval-shaped area of the retina that is referred to as the “MacTel zone”, see Figure 1. The MacTel zone is centered on the part of your retina that is responsible for allowing us to see fine details. This central portion of the retina containing the MacTel zone is part of the macula.
These changes can be documented using a fundus camera that takes a picture of the back of your eye. Examples of findings described above are shown in Figure 1.
Figure 1: Color fundus photographs of a healthy person and three patients with MacTel. In eyes with MacTel, changes are usually limited to a central, oval-shaped area, called “MacTel zone” that is centered on the fovea and located within the macular area. Changes usually start within a region called “temporal parafovea” (a smaller area, next to the fovea, located on the opposite side to the optic nerve head). Your eye doctor will look within this region for changes that are characteristic of MacTel.
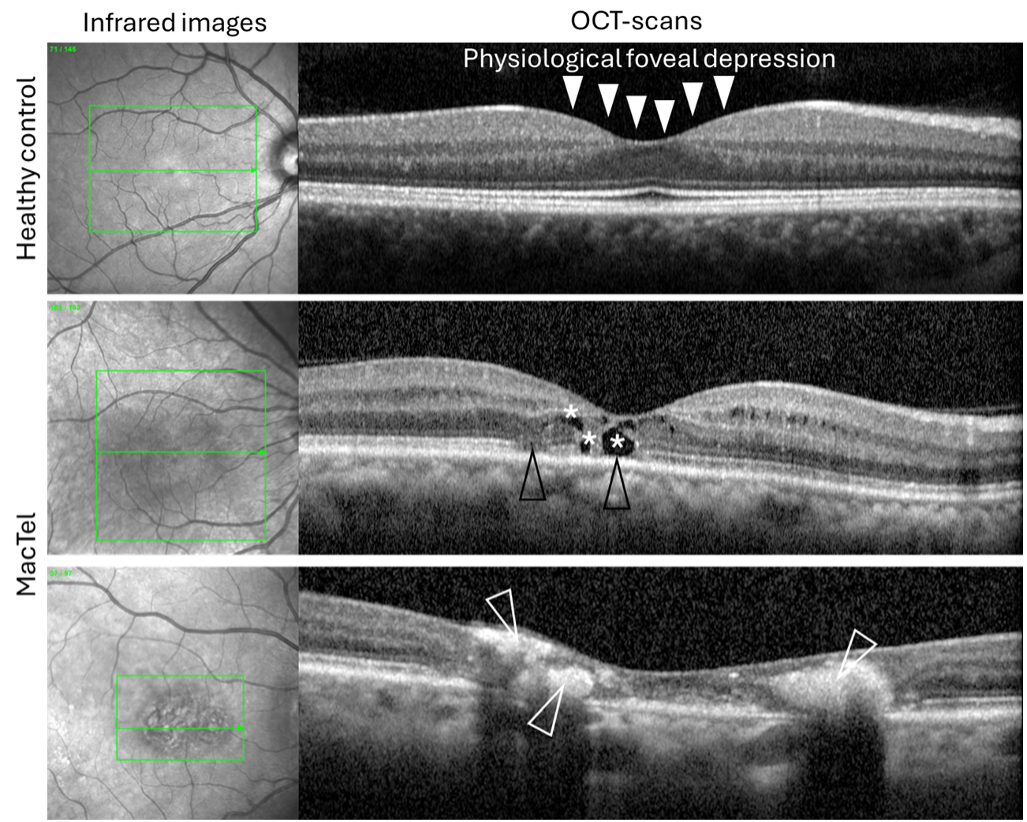
An important diagnostic and monitoring tool in MacTel is the optical coherence tomography (OCT) scan of the macular area. The OCT scan results in very high-resolution images, and the doctor can “look inside” your retina with a cross-sectional view (e.g. they can look at the layers of your retina from the side-view, see Figure 2). For this test, you will rest your forehead and chin on the device, but this time you will be looking into the machine while it scans your eye. Your eye doctor will look for structural changes, including:
– “Cysts” (little cavities within your retina)
– Disruptions of certain retinal layers (mainly the layers where our photoreceptors – rods and cones – are located)
– Changes that show an increased reflectivity signal (“hyper-reflective changes” that have been shown to represent vascular changes and/or migrating/growing pigment).
– Rarely, neovascularization (see description above) may be seen.
OCT scans are commonly performed at most visits. Examples for OCT scans in healthy eyes and eyes with MacTel are shown in Figure 2.
Figure 2: Retinal optical coherence tomography (OCT) scans of a healthy eye (top row), compared to two eyes with MacTel (bottom two rows). The infrared image on the left side (under “Infrared images”) helps your doctor determine where each OCT-scan is located in the back of your eye. In MacTel, little cysts (in this example they are indicated with stars), disruptions of retinal layers (mainly layers containing the photoreceptors; black arrowheads) or hyper-reflective changes (here illustrated in white; white arrowheads; see main text for details) may be seen. Note the healthy eye showing a physiological foveal depression (your fovea is the small depression in the center of your macula (solid white arrowheads), where visual acuity is the highest) and retinal layers are smooth and uninterrupted.
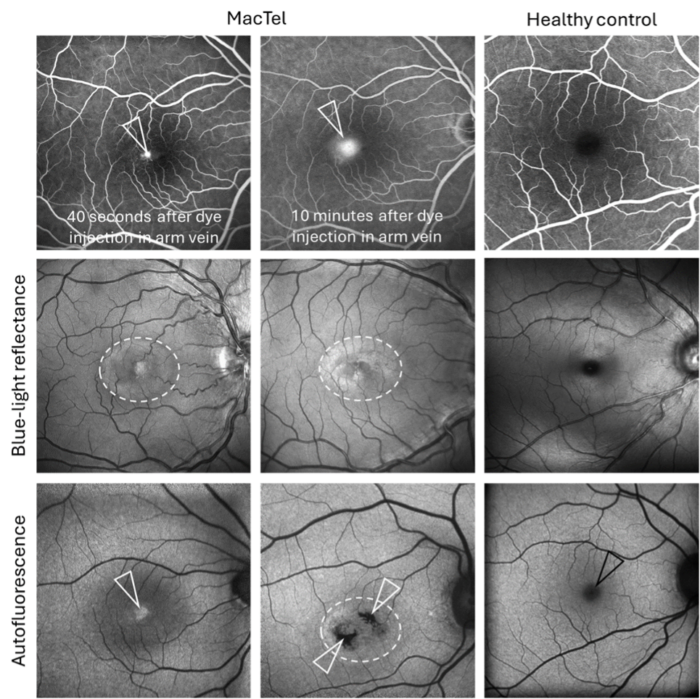
Another imaging exam you can expect to have done is a fundus autofluorescence image. This is an imaging technique that maps “fluorophores” (fluorophores are naturally and pathologically occurring molecules that absorb and emit light of particular wavelengths) in the posterior pole of your eye. For this exam, a fundus camera equipped with certain light sources and filters will shine a light into the eye and capture a picture of the resulting fundus autofluorescence. The doctor will look for areas of increased or decreased autofluorescence, compared to what they expect to see in a healthy eye, see Figure 3.
A blue light reflectance image may also be captured. For this test, a blue light is shined into the eye, where it is absorbed and reflected differently by retinal tissues. The pattern of blue light reflectance from a MacTel retina will differ in comparison to a healthy retina, see Figure 3.
Lastly, your eye doctor will perform an exam called fluorescein angiography. For this exam, a dye will be injected into your arm vein, and a photographer will take multiple images of both eyes using a bright blue light. These pictures give your eye doctor a view of the vessels in the back of your eyes, and how the dye travels through those vessels. They will be able to see any structural abnormalities of the vessels (abnormal, dilated vessels, called “telangiectasia”), and whether the dye leaks out of any of your vessels, which is typical for MacTel. Rarely, they may see neovascularization (see description above). This test is usually only performed at one of your initial visits and only repeated if needed. Example images are shown in Figure 3.
Figure 3: Fluorescein angiography (top row): Vessels are filled with dye (white). In eyes with MacTel, small vessels may be dilated and leaky. Note how the dye leaks out of small central vessels, and leakage increases over time (from 40 seconds to 10 minutes after injecting the dye; white arrow heads). Blue-light reflectance: Changes in signaling (here an increased signal; areas within an oval-shaped central area (dotted lines) appear “lighter”, compared to the healthy eye without MacTel. Autofluorescence: Changes in signaling (either increased (“white”) or decreased (“black”) areas may be noted in the center (see white arrowheads). Note how these changes compare to a healthy control eye, showing a central physiological “dark spot” (black arrowhead) which represents the normal peak of the macular pigment.
Based on the findings on different imaging modalities and the fundus exam, your doctor will be able to determine the current stage of disease for each eye. They will also be able to document disease progression over time, by comparing results of the current visit to results from previous visits, looking for signs of disease progression.
The office visit exams described here might be expected at an eye doctor visit, or as part of a MacTel Project Natural History and Observation Registry (NHOR) enrollment visit. The NHOR study does not generally entail follow-up visits, so you should continue to be followed by your regular eye doctor. Your doctor will determine how often you need to be seen for MacTel.